Medical bodies say thin surgical masks do not provide adequate protection for frontline personnel
The Guardian
Denis Campbell Health policy editor
Mon 27 Dec 2021
The FFP3 face mask is much more effective but expensive. The Department of Health and Social Care only recommends their use in limited circumstances. Photograph: Victoria Jones/PA
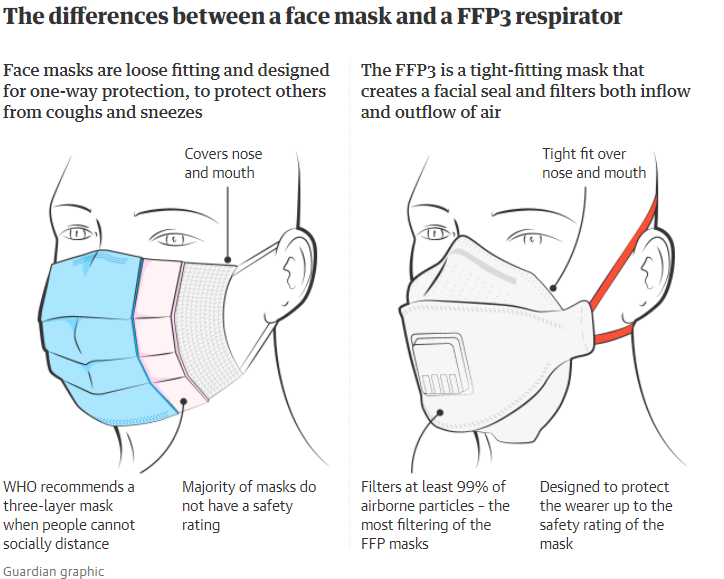
NHS staff treating Covid patients should be given much more protective facewear than thin surgical masks to help them avoid getting infected during the Omicron rise, doctors say.
The British Medical Association (BMA), Hospital Consultants and Specialists Association (HCSA) and Doctors’ Association UK are calling for frontline personnel to be given FFP3 masks.
Making the much higher-quality face masks standard issue would save the lives of health workers who fall ill as a result of treating Covid patients, the BMA said. “At this critical point in the pandemic this is extremely urgent — a matter of life and death,” said Prof Raymond Agius, the acting chair of the doctors’ union’s occupational health committee.
FFP3 masks, also known as filtering facepiece respirators, have been shown in a trial in Addenbrooke’s hospital in Cambridge to reduce the number of healthcare staff who become infected.
However, the Department of Health and Social Care’s (DHSC) guidance on personal protective equipment, updated last week, only recommends their use in limited circumstances.
“With a high transmissible new strain now circulating, and clear evidence that Covid-19 spreads in small airborne particles, healthcare workers must be given the best possible protection against the virus. Surgical masks don’t give the necessary protection against airborne transmission of Covid,” Agius said.
The BMA has written to every hospital trust in England demanding that any health professional treating patients who are or may be Covid-positive should be routinely issued with FFP3s, which are much more expensive than the surgical masks usually provided.
Surgical masks are “unsuitable” given the threat Covid poses, the BMA believes.
In its letter it has reminded hospital chief executives of their legal responsibilities as employers to keep their staff safe from harm, including by providing FFP3s.
A handful of hospitals are understood to already issued FFP3 respirators as standard, but most do not.
Dr Claudia Paoloni, the president of the HCSA, said that giving staff proper PPE would help reduce the fast-growing tide of sickness absence among frontline workers who are getting Covid.
“If we don’t get PPE right we risk contributing to a further wave of sickness absences when hospitals and patients can least afford it.
“The current reliance on inadequate fluid-resistant surgical masks is likely to leave staff vulnerable in enclosed hospital settings,” Paoloni said.
“The fear, as in 2020, is that we are seeing a cavalier approach to safety where infection control guidelines are once again being driven by supply issues and cost.
“We need hospitals to see sense and take a precautionary approach,” by making FFP3s available to anyone who wants to use one instead of a surgical mask, Paoloni added.
The BMA has also written to NHS England asking it to ensure all GP practices are also issued with FFP3s instead of surgical masks, particularly because family doctors often work in small, cramped surgeries.
“Healthcare workers in hospitals and GP surgeries are putting themselves and potentially their own families at risk, particularly with this new, highly transmissible Omicron variant,” said Dr Vishal Sharma, the chair of the BMA’s pensions committee.
The DHSC’s updated guidance, published last Tuesday, says “staff should assess any likely blood and body fluid exposure risk and ensure PPE is worn that provides adequate protection against the risks associated with the procedure or task being undertaken”. However, it only advises frontline staff to use an FFP3 if they are undertaking an aerosol-generating procedure, such as intubating a patient who is going on to a mechanical ventilator, and not with Covid patients generally.
A DHSC spokesperson confirmed that it does not plan to recommend routine use of FFP3 masks.
“The safety of the NHS and social care staff has always been our top priority and we continue to deliver PPE to protect those on the frontline.
“Guidance on the appropriate levels and standards of PPE is written by clinical experts. Updated infection prevention control guidance was published this month to reflect the latest scientific understanding on how to prevent transmission of Covid-19.
“Emerging evidence and data are continually monitored and reviewed and guidance will be amended accordingly if appropriate.”
Originally published at https://www.theguardian.com on December 27, 2021.
Names cited
Prof Raymond Agius, the acting chair of the doctors’ union’s occupational health committee.
The British Medical Association (BMA), Hospital Consultants and Specialists Association (HCSA) and Doctors’ Association UK
Dr Claudia Paoloni, the president of the HCSA
ORIGINAL PUBLICATION

FFP3 respirators protect healthcare workers against infection with SARS-CoV-2
Mark Ferris, Rebecca Ferris,Chris Workman,Eoin O’Connor,David A Enoch,Emma Goldesgeyme,Natalie Quinnell,Parth Patel,Jo Wright,Geraldine Martell,Christine Moody,Ashley Shaw,Christopher J.R. Illingworth,Nicholas J. Matheson,Michael P. Weekes
COMMENTS TO THE ORIGINAL PUBLICATION

News
Covid-19: Upgrading to FFP3 respirators cuts infection risk, research finds
BMJ 2021; 373 doi: https://doi.org/10.1136/bmj.n1663 (Published 29 June 2021)Cite this as: BMJ 2021;373:n1663
Jacqui Wise, Kent, UK
News
Covid-19: Upgrading to FFP3 respirators cuts infection risk, research finds
BMJ 2021; 373 doi: https://doi.org/10.1136/bmj.n1663 (Published 29 June 2021)Cite this as: BMJ 2021;373:n1663
Jacqui Wise, Kent, UK
Upgrading face masks to filtering face piece (FFP3) respirators for healthcare workers on covid-19 wards produced a dramatic reduction in hospital acquired SARS-CoV-2 infections, according to research carried out at Addenbrooke’s Hospital in Cambridge.1
The study, published as a preprint, has been welcomed by campaigners who have been calling on the government to ensure that healthcare workers are given better personal protective equipment (PPE).
For most of last year Cambridge University Hospitals NHS Foundation Trust followed national guidance that healthcare workers should use fluid resistant surgical masks as respiratory protective equipment unless aerosol generating procedures (AGPs) were being carried out when FFP3 respirators were advised.
Since the start of the pandemic the trust has been regularly screening its healthcare workers for SARS-CoV-2 even when asymptomatic. They found that healthcare workers on “red” covid-19 wards were at greater risk of infection than staff on “green” wards even when using the recommended protective equipment. So in December 2020 the trust implemented a change in policy so that staff on red wards wore FFP3 masks instead of fluid resistant surgical masks.
Before the change in policy, cases among staff were higher on covid-19 wards compared with non-covid-19 wards in seven out of eight weeks analysed. Following the change in protective equipment the incidence of infection on the two types of ward was similar. Of 609 positive results over the eight week study period, 169 were included in the study. Those excluded were healthcare workers who were not ward based or worked between different wards, non-clinical staff, and staff working in critical care areas.
The researchers developed a simple mathematical model to quantify the risk of infection for healthcare workers. This found that the risk of direct infection from working on a red ward before the change in policy was 47 fold greater than the corresponding risk from working on a green ward. While almost all cases on green wards were likely caused by infection in the community, cases on red wards at the beginning the study period were attributed mainly to direct, ward based exposure.
The model also suggested that the introduction of FFP3 respirators provided 100% protection (confidence interval 31.3%, 100%) protection against direct, ward based covid infection.
The research was funded by Wellcome, the Addenbrooke’s Charitable Trust, UK Research and Innovations, and the NIHR Cambridge Biomedical Research Centre.
Study author, Chris Illingworth from the MRC Biostatistics Unit at the University of Cambridge, said, “Before the face masks were upgraded, the majority of infections among healthcare workers on the covid-19 wards were likely because of direct exposure to patients with covid-19. Once FFP3 respirators were introduced, the number of cases attributed to exposure on covid-19 wards dropped dramatically — in fact, our model suggests that FFP3 respirators may have cut ward based infection to zero.”
Michael Weekes from the department of medicine at the University of Cambridge, added, “Our data suggest there’s an urgent need to look at the PPE offered to healthcare workers on the frontline. Upgrading the equipment so that FFP3 masks are offered to all healthcare workers caring for patients with covid-19 could reduce the number of infections, keep more hospital staff safe, and remove some of the burden on already stretched healthcare services caused by absence of key staff because of illness.
The BMA, the Royal College of Nursing, and other professional bodies have been calling for some time for FFP3 masks to be provided more widely. In January 2021 FreshAir NHS, a group of frontline NHS workers, wrote an open letter to all UK governments requesting airborne mitigations to prevent infections in healthcare staff and reduce nosocomial infection risk to patients.2 In a BMJ Opinion piece, the group welcomed the new data, saying it provided yet more evidence of why the policy needs to change.3
Public Health England recently updated its guidance to oblige NHS organisations to assess the risk that covid-19 poses to staff and provide FFP3 respirators where appropriate and not just when AGPs are taking place.45 The update follows a review by the government’s Scientific Advisory Group for Emergencies published in April which said that the decision to use FFP3 respirators should be based on a risk assessment that considers the interaction with a patient, the duration and proximity of exposure, whether there is good fitting and mask adherence, whether staff are routinely wearing eye protection, and whether patients wear masks.6
This article is made freely available for use in accordance with BMJ’s website terms and conditions for the duration of the covid-19 pandemic or until otherwise determined by BMJ. You may use, download and print the article for any lawful, non-commercial purpose (including text and data mining) provided that all copyright notices and trade marks are retained.
References
↵Ferris M, Ferris R, Workman C, et al. FFP3 respirators protect healthcare workers against infection with SARS-CoV-2.Authorea [Preprint]. 2021doi:10.22541/au.162454911.17263721/v1.CrossRefGoogle Scholar
↵Wise J. Covid-19: Doctors and nurses demand better PPE for wider range of procedures. BMJ2021;372:n30. doi:10.1136/bmj.n30 pmid:33408072FREE Full TextGoogle Scholar
↵Lawton T, Butler M, Peters C, et al. Use of airborne precautions for covid-19 in healthcare settings. BMJ Opinion. 28 June 2021. https://blogs.bmj.com/bmj/2021/06/28/use-of-airborne-precautions-for-covid-19-in-healthcare-settings.
↵Public Health England. Covid-19: guidance for maintaining services within health and care settings. 2020. www.gov.uk/government/publications/wuhan-novel-coronavirus-infection-prevention-and-control
↵Torjesen I. Covid-19: PPE guidance is upgraded as evidence of airborne transmission grows. BMJ2021;373:n1422. doi:10.1136/bmj.n1422 pmid:34078639FREE Full TextGoogle Scholar
↵SAGE. Masks for healthcare workers to mitigate airborne transmission of SARS-CoV-2. 25 March 2021. www.gov.uk/government/publications/emg-masks-for-healthcare-workers-to-mitigate-airborne-transmission-of-sars-cov-2-25-march-2021.