Health Leaders Media
CHRISTOPHER CHENEY
SEPTEMBER 20, 2021
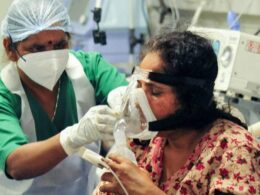
Telediagnosis on the grand scale experienced since the beginning of the coronavirus pandemic is an evolving science, researchers find.
More research is necessary to ensure diagnostic quality and safety in telemedicine, a new report published by the Society to Improve Diagnosis in Medicine (SIDM) says.
Telemedicine utilization has expanded exponentially since the beginning of the coronavirus pandemic. As noted in the new report, most research on telemedicine has focused on the maintenance health, but the use of telemedicine for telediagnosis at a grand scale is not as well understood.
The new report, which is based on information collected from healthcare organizations, clinicians, vendors, and patients, includes several key findings.
- Remote patient monitoring is “an important enabler of continuity of care and patient support” in telemedicine that can facilitate diagnostic quality and safety.
- Many clinicians interviewed for the report said that the skillset necessary for a good diagnosis in an in-person visit is similar to the skillset necessary to make a good telediagnosis.
- Clinicians reported that a primary barrier in telediagnosis is the inability to perform a physical exam.
- A crucial area for more research is in determining when a virtual visit is appropriate and when an in-person visit is necessary.
- Many patients interviewed for the report had developed their own triage framework for determining when a telemedicine visit is appropriate.
For example, patients said they would be comfortable with a telemedicine visit to assess familiar symptoms such as a recurring earache.
Insights from the report
- Remote patient monitoring has significant potential to improve telediagnosis quality and safety, Suzanne Schrandt, JD, a co-author of the report and senior patient engagement advisor at SIDM, told HealthLeaders.
“We talked with a number of folks involved in remote patient monitoring, including vendors and clinicians who use those services. It seems to have a great deal of promise, particularly for early detection in an otherwise healthy person who has new symptomology or in a person with an underlying health condition who starts to see some worrisome changes,” she said.
- Remote patient monitoring can also boost patient engagement, Schrandt said.
“One of the things that jumped out to me is there seems to be some value from remote patient monitoring in keeping the patient engaged and active in their own care. Patients can be aware of their own symptomology, vital signs, and any other measurements that are captured.”
- The inability to conduct a physical exam can be problematic in telediagnosis, she said.
“What we heard from the 50 listening sessions is that the most important thing is the presenting symptoms. Clearly, there are some symptoms that do not require a physical exam; and in that case, most clinicians and patients felt comfortable with the virtual care. But there are trickier, more amorphous symptoms that require a physical exam such as abdominal pain and swelling that are difficult to perceive over a camera.”
- Clinicians interviewed for the report said they had found innovative ways to avoid the need to conduct a physical exam, Schrandt said.
“We heard many great examples from the clinicians we talked to about things that they figured out in the moment. One was assessing strength over the camera by asking the patient to pick up increasingly heavy objects as opposed to assessing strength in a physical exam by pressing down on limbs.
Clinicians can also ask patients to do their own self-exam while the doctor is watching, so they could isolate an area of pain or an area of discomfort.”
- Equipping patients with simple diagnostic instruments can also obviate the need to conduct a physical exam, she said.
“There are some great opportunities to figure out how instruments such as oximeters and blood pressure cuffs can be used by patients to supplement when a clinician cannot do a physical exam.”
- When asked about the skillsets needed to conduct telediagnosis versus diagnosis in person, clinicians interviewed for the report had two opposing responses, Mark Graber, MD, report co-author and SIDM president emeritus, told HealthLeaders.
“One was that the same skills you use to be effective in person would help you be effective virtually. The opposing view was that telediagnosis was a whole new ballgame, with new rules, new tools, and new everything. Those with the opposing view said that virtual care did not come naturally, that there was a learning curve, and that instruction and practice and feedback were valuable. Someone even mentioned having done simulated sessions to get up to speed, and that this experience was valuable,” he said.
Conducting a virtual visit and a physical exam are different in many ways, Graber said.
“A simple example is the ongoing debate on how to evaluate someone who is short of breath. This is a piece of cake in person-you see how fast the patient is walking, whether they are pale or blue, how fast and how heavy they are breathing, and you probably already have a set of vital signs taken that include the respiratory rate, the heart rate, and even a pulse oximeter reading if you are lucky.
Contrast that to the virtual encounter, where you may get the same short-of-breath complaint, but there is ongoing debate about how you evaluate this,” he said.
In-person visits versus virtual visits
The report found there are five decision factors when deciding whether a patient should have an in-person visit or a telemedicine visit, Schrandt said.
- “The first decision factor is the urgency of symptoms.
There are some symptoms that warrant immediate, in-person attention such as chest pain. There are some symptoms that are clearly nonurgent such as a rash. However, what about the gray area?
A patient could have a symptom that is unusual, but it is hard to determine the urgency. We need more research on methods for making those sorts of determinations. We need to know from the clinical perspective and the patient perspective what constitutes urgency.”
- “The second decision factor is the underlying health of the patient.
Is this a chronic disease patient with very specific risk factors at play, or is this an otherwise healthy person?
We need research to determine whether there are conditions that are going to require in-person assessment.”
- “The third decision factor is the familiarity of the symptoms.
Is this the same earache you have had five times or is this a new symptom you have never experienced? We might be able to develop an algorithm tool that could flag when there is a symptom that calls for an in-person visit and when it is probably OK to do virtual care. We need much more research on that.”
- “The fourth decision factor is the relationship between the patient and the provider. This can get complicated.
If there is a well-established relationship, there could be more comfort with virtual care, or at least a virtual-first approach.
On the flip side, a patient can be matched with a clinician in telemedicine who the patient does not know, and we need research to know whether there are situations where that model works well or whether there are certain scenarios when that is not the right approach.”
- “The fifth decision factor is the quality of the virtual care.
Is the visit being done over the phone? If the visit is being conducted via video, is the quality of the video clear? The concern over inequity and access to broadband came up repeatedly during the project. You cannot make decisions about whether to have in-person visits or virtual visits unless the virtual is an option.”
Names cited:
Suzanne Schrandt, JD, a co-author of the report and senior patient engagement advisor at SIDM;
Mark Graber, MD, report co-author and SIDM president emeritus;
Originally published at https://www.healthleadersmedia.com.