Time
Monday, June 28, 2021
BY ALEX FITZPATRICK
To Boost, or Not to Boost?
Based on medical trials and real-world data, we know that the COVID-19 vaccines authorized for use in the United States are safe and highly effective.
But for the roughly half of Americans (and hundreds of millions of people around the world) inoculated so far, a couple big, unanswered questions remain: will we need booster shots, and if so, when?
Those have been difficult questions to answer, in part because time travel hasn’t been invented yet. The first study participants to receive the vaccines got their shots just over a year ago, meaning limited long-term efficacy data are available.
So far, much of that data suggest that, yes, those who have been vaccinated will need a booster shot, perhaps fairly soon. “I think as we get into the fall, we’re going to have to look at giving, especially the vulnerable population, boosters,” former U.S. Food and Drug Administration boss Dr. Scott Gottlieb said on CNBC earlier this month; other experts generally share a similar view.
However, a study published in the journal Nature this morning points to a different conclusion: the Pfizer-BioNTech and Moderna vaccines, both of which are based on mRNA technology, may protect recipients against the coronavirus for years.
In the study, researchers extracted samples of lymph fluid from 14 Pfizer vaccine recipients several times over the course of nearly four months.
They found that specialized immune cells were still being trained to fight off the coronavirus 15 weeks after inoculation.
That process usually ends about a month after vaccination, one of the study’s authors told the New York Times, suggesting that the mRNA vaccines provide long-lasting protection. (The study didn’t look at the Janssen/Johnson & Johnson vaccine.)
While this study is promising, it’s far from the end of the booster discussion.
The virus that causes COVID-19 is already mutating — you’ve probably heard of the Delta and Delta Plus variants — and while the current vaccines seem mostly effective against the current variants, a new version may yet emerge that more successfully evades existing inoculations.
Meanwhile, public health officials may take a cautious route and advise that people who are particularly vulnerable to COVID-19, like the elderly and those with certain pre-existing conditions, get a booster just to be safe.
Personally, I’m mentally preparing to get a booster this fall along with my flu shot to help my body fight off both viruses as winter sets in.
Originally published at time.com

Pfizer and Moderna Vaccines Are Likely to Produce Long-Lasting Immunity, Study Suggests
New York Times
June 28th, 2021
Close examinations of more than a dozen vaccinated people found that immune cells were still organizing to fight the coronavirus months after inoculation.
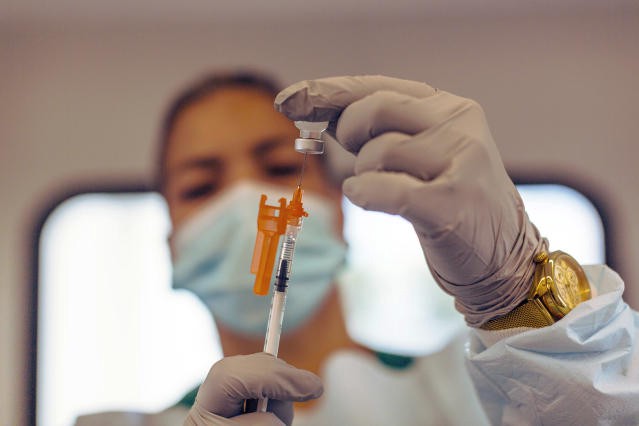
A health care worker prepares to administer the Pfizer Covid-19 vaccine at a vaccination event last month in Miami. Credit… Saul Martinez for The New York Times

The vaccines made by Pfizer-BioNTech and Moderna set off a persistent immune reaction in the body that may protect against the coronavirus for years, scientists reported on Monday.
The findings add to growing evidence that most people immunized with the mRNA vaccines may not need boosters, so long as the virus and its variants do not evolve much beyond their current forms — which is not guaranteed. People who recovered from Covid-19 before being vaccinated may not need boosters even if the virus does make a significant transformation.
“It’s a good sign for how durable our immunity is from this vaccine,” said Ali Ellebedy, an immunologist at Washington University in St. Louis who led the study, which was published in the journal Nature.
The study did not consider the coronavirus vaccine made by Johnson & Johnson, but Dr. Ellebedy said he expected the immune response to be less durable than that produced by mRNA vaccines.
Dr. Ellebedy and his colleagues reported last month that in people who survived Covid-19, immune cells that recognize the virus lie quiescent in the bone marrow for at least eight months after infection. A study by another team indicated that so-called memory B cells continue to mature and strengthen for at least a year after infection.
Based on those findings, researchers suggested that immunity might last for years, possibly a lifetime, in people who were infected with the coronavirus and later vaccinated. But it was unclear whether vaccination alone might have a similarly long-lasting effect.
Dr. Ellebedy’s team sought to address that question by looking at the source of memory cells: the lymph nodes, where immune cells train to recognize and fight the virus.
After an infection or a vaccination, a specialized structure called the germinal center forms in lymph nodes. This structure is an elite school of sorts for B cells — a boot camp where they become increasingly sophisticated and learn to recognize a diverse set of viral genetic sequences.
The broader the range and the longer these cells have to practice, the more likely they are to be able to thwart variants of the virus that may emerge.
“Everyone always focuses on the virus evolving — this is showing that the B cells are doing the same thing,” said Marion Pepper, an immunologist at the University of Washington in Seattle. “And it’s going to be protective against ongoing evolution of the virus, which is really encouraging.”
After infection with the coronavirus, the germinal center forms in the lungs. But after vaccination, the cells’ education takes place in lymph nodes in the armpits, within reach of researchers.
Dr. Ellebedy and his colleagues recruited 41 people — including eight with a history of infection with the virus — who were immunized with two doses of the Pfizer-BioNTech vaccine. From 14 of these people, the team extracted samples from the lymph nodes at three, four, five, seven and 15 weeks after the first dose.
That painstaking work makes this a “heroic study,” said Akiko Iwasaki, an immunologist at Yale. “This kind of careful time-course analysis in humans is very difficult to do.”
Dr. Ellebedy’s team found that 15 weeks after the first dose of vaccine, the germinal center was still highly active in all 14 of the participants, and that the number of memory cells that recognized the coronavirus had not declined.
“The fact that the reactions continued for almost four months after vaccination — that’s a very, very good sign,” Dr. Ellebedy said. Germinal centers typically peak one to two weeks after immunization, and then wane.
“Usually by four to six weeks, there’s not much left,” said Deepta Bhattacharya, an immunologist at the University of Arizona. But germinal centers stimulated by the mRNA vaccines are “still going, months into it, and not a lot of decline in most people.”
Dr. Bhattacharya noted that most of what scientists know about the persistence of germinal centers is based on animal research. The new study is the first to show what happens in people after vaccination.
The results suggest that a vast majority of vaccinated people will be protected over the long term — at least, against the existing coronavirus variants. But older adults, people with weak immune systems and those who take drugs that suppress immunity may need boosters; people who survived Covid-19 and were later immunized may never need them at all.
Exactly how long the protection from mRNA vaccines will last is hard to predict. In the absence of variants that sidestep immunity, in theory immunity could last a lifetime, experts said. But the virus is clearly evolving.
“Anything that would actually require a booster would be variant-based, not based on waning of immunity,” Dr. Bhattacharya said. “I just don’t see that happening.”
People who were infected with the coronavirus and then immunized see a major boost in their antibody levels, most likely because their memory B cells — which produce antibodies — had many months to evolve before vaccination.
The good news: A booster vaccine will probably have the same effect as prior infection in immunized people, Dr. Ellebedy said. “If you give them another chance to engage, they will have a massive response,” he said, referring to memory B cells.
In terms of bolstering the immune system, vaccination is “probably better” than recovering from the actual infection, he said. Other studies have suggested that the repertoire of memory B cells produced after vaccination is more diverse than that generated by infection, suggesting that the vaccines will protect better against variants than natural immunity alone.
Dr. Ellebedy said the results also suggested that these signs of persistent immune reaction might be caused by mRNA vaccines alone, as opposed to those made by more traditional means, like Johnson & Johnson’s.
But that is an unfair comparison, because the Johnson & Johnson vaccine is given as a single dose, Dr. Iwasaki said: “If the J & J had a booster, maybe it will induce this same kind of response.”
Originally published at https://www.nytimes.com on June 28, 2021.